How did pandemic-era ACA subsidies work, and why did they expire? Analyst Notes
Go behind the scenes with our team as we find and make sense of the numbers.
Americans care a lot about the cost of healthcare — in fact, there’s more interest now, than ever* (*Ever, according to 24 years of internet search-based activity).
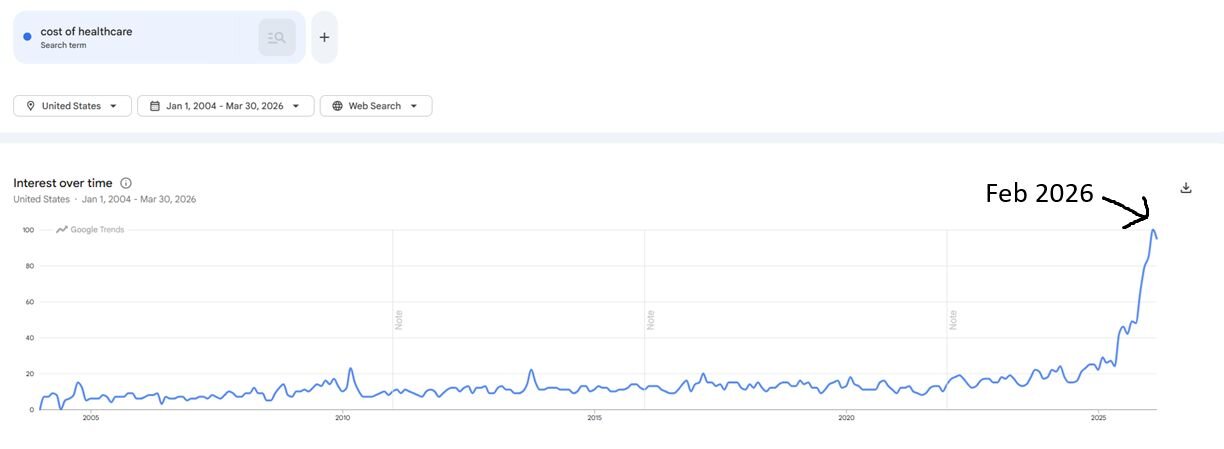
Measured on a scale where 0 equals no interest and 100 equals highest interest ever, the term “cost of healthcare” reached its peak interest level on Google in February 2026.
That interest is understandable: healthcare costs are also higher than ever. Personal healthcare spending has increased nearly every year since 1980. Adjusted for inflation, healthcare costs were 3.7 times higher in 2024 than in 1980.
Inflation-adjusted per person healthcare spending was 3.7x higher in 2024 vs. 1980.
Per-capita personal healthcare spending, 1980–2024
And what else has been on people’s minds? The end of pandemic-era provisions that subsidized healthcare costs related to the Affordable Care Act (ACA). (It was part of the reason the government shut down late last year!) I wrote an extensive article about the whys and hows of these provisions, and even then I couldn't answer all the questions I had. Why? Let’s peek behind the data curtain.
In 2010, Congress passed the Affordable Care Act (ACA) with the intention of reducing healthcare costs and expanding coverage, (especially for those who don’t have employer-based insurance and don’t qualify for other programs like Medicare or Medicaid).
For many Americans, ACA-qualified marketplace plans and subsidies are an answer to cost and accessibility: in 2025, about 24.3 million Americans were enrolled in qualified marketplace plans (around 7.2% of the population). Of those enrollees, 92.2% received subsidy assistance.
ACA-qualified marketplace plan enrollment more than doubled in from 2020 to 2025.
But enrollment looked pretty different in 2020, around 11.4 million people were accessing healthcare via qualified health plans. In other words, enrollment more than doubled from 2020 to 2025. That’s a big shift, especially compared to the five year span prior (2015-2019). Back then, qualified plan enrollment didn’t waver much: it hit a high of 12.7 million enrollees in 2016, and a low of 11.4 million in 2019.
There were shifts on the subsidy side, too: In 2020, 84.3% of marketplace enrollees received a subsidy that made their monthly premiums more affordable. By 2025, 92.2% did. Remember, too, that the number of people with plans nearly doubled, so not only did the percentage of people receiving subsidies increase (from 84.3% to 92.2%), but so did the number (9.6 million to 22.4 million).
ACA consumers receiving APTC increased 133% from 2020 to 2025.
Number of ACA consumers with an without APTC
So why did enrollments go up?
Before we get too much further, let’s review some terminology (or if you’re a Smarty McSmarterson and don’t need a refresher, I’ll see you in the next section). Here are some foundational concepts about qualified plans and subsidies:
ACA Marketplace: The ACA established the Health Insurance Marketplace, or “ACA Marketplace,” as a platform where individuals and families can shop for and enroll in private, ACA-certified insurance plans. The ACA Marketplace’s purpose is to provide an insurance option for people who don't have insurance through an employer (like freelancers, people between jobs, part-time workers), or through a public program such as Medicaid or Medicare. Depending on the state the enrollee lives in, plans are hosted one of three ways:
- State-based exchanges/State-based marketplace (SBE/SBM): In this marketplace, states run all functions of the marketplace, and have their own systems for evaluating eligibility, managing enrollment, and supporting enrollees.
- Healthcare.gov (HC.gov): This is a federally facilitated website that operates in states where states have chosen not to make their own marketplace.
- State-based using a federal platform: In this scenario, the state is responsible for conducting all usual business for an individual marketplace but relies on the federal exchange for eligibility and enrollment functions.
By default, states use the HC.gov option unless they opt into the SBE option by declaring intent to host a state-based platform, and by getting approval from the Centers for Medicare and Medicaid Services.
Here is a map of which states use which system. In 2025, over half (31 states) used HC.gov, while 19 states and Washington, DC, used SBE.
Most states use the federal HealthCare.gov marketplace.
States by marketplace type, 2025
Qualified health plan: Qualified health plans are insurance plans certified by the Health Insurance Marketplace that comply with ACA requirements, including covering essential health benefits, meeting cost-sharing limits, and prohibiting denial of coverage based on pre-existing conditions.
Subsidies: While ACA Marketplace plans are available to most people regardless of income, the ACA offers income-based subsidies to eligible enrollees to make monthly premiums more affordable. These are two ways qualified enrollees can receive this assistance: cost-sharing reductions (CSRs) or Advance Premium Tax Credits (APTCs).
- Cost-sharing reductions make out-of-pocket costs, such as deductibles, copayments, and coinsurance, cheaper for enrollees. They also reduce the most a patient must pay for covered services before insurance pays for 100% of all covered services.
- Premium Tax Credits lower the monthly cost of ACA Marketplace health insurance. These credits are often delivered in advance as Advance Premium Tax Credits (APTCs), which are paid directly to insurance companies by the federal government on behalf of enrollees, reducing enrollees’ monthly premium costs.
To recap: the ACA created Marketplace, which is where enrollees sign up for qualified health plans, and where some enrollees can get subsidies in the form of CSRs and/or APTCs. (You’re probably prettyyy glad we did a terminology review).
Okay, I understand all that. So, why did enrollments go up?
In 2021, as a protection against Americans losing healthcare due to job losses related to the pandemic, Congress introduced the American Rescue Plan Act which temporarily (more on this in a sec) broadened the existing criteria to receive APTCs, making more people eligible for them. And it called them... Enhanced Premium Tax Credits.
Think of it like Super Mario: APTCs are like little Mario, the American Rescue Plan Act of 2021 is the mushroom that makes him grow, and the enhanced Premium Tax Credits are like big Mario. They’re the same thing, one’s not better than the other, but they have different capabilities.
Mario image via X.com. We added the APTC text.
If you’re thinking “But big Mario can shrink back to little Mario... can Enhanced Premium Tax Credits return to APTCs?” Excellent question. A portent of things to come. But if you’re thinking “isn’t a mushroom more like an extra life for Mario?” well, this mushroom/Mario thing is a close but imperfect metaphor.
Anyway! Back to Enhanced Premium Tax Credits.
These credits expanded APTCs in two ways:
- It removed the APTC income caps. Before the enhancement, eligibility was limited to households with incomes at or above 100% of the federal poverty level (FPL), and no more than 400% of the FPL. The enhancement removed the 400% component from the equation, leaving 100% as the only income threshold.
- It limited household healthcare premium contributions to 8.5% of income, reducing how much enrollees paid each month for Marketplace plans. The original ACA used a sliding scale of “applicable percentages” tied to income as a share of the federal poverty level. In other words, an enrollee’s contribution amount is the product of their household income and an applicable percentage that increases as household income increases. In practice, this meant contributions ranged roughly from 2% of income at the low end (around 100–133% FPL) up to approximately 9.5% of income at the top end (around 300–400% FPL), with the percentages increasing gradually.
These two changes, in tandem with pandemic-related job losses (which meant losing employer-based healthcare), led to people both enrolling in qualified marketplace plans and qualifying for subsidy payment assistance.
Can we tell how the enhancements affected what people paid for ACA plans each month?
Kind of, but not as directly as we would like. Let’s start with why we couldn’t make a direct high-level comparison of what people were paying on average in 2025 versus 2020.
I found that in 2025, among enrollees who received the APTC subsidy, enrollees paid a monthly average of $74 dollars for their premium, and the monthly amount of APTC subsidy they received was $550. So far, so good.
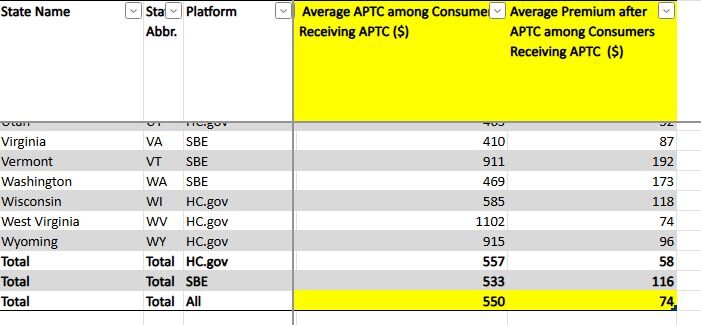
And in 2020, before the expansion, enrollees receiving APTC subsidies paid a monthly average of... darn, that data wasn't available. Where I expect the average value to be, it says “NR.”
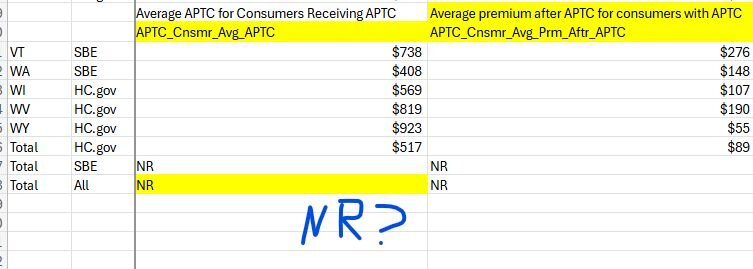
The term “NR” isn’t defined in the Centers for Medicare and Medicaid Services data files, nor is it in the definition file it provides for the dataset. A quick Google search shows that “NR” can be an acronym for many things, so I’m not sure exactly what it means. “AI Thought Partner” Claude had a few ideas, including “not reported”:

To get the national “total” value, it looks like the “total” for the HC.gov and SBE states must be present. In this case, the “total” is something like an average, although I’m not sure exactly what that calculation is (I do know it’s not a mean average). Looks like the 2020 HC.gov total is available, but SBE value isn’t. (Also, not sure why this value is called “total” in the dataset when it’s definitely not a sum...)
I suspect this is because, in 2020, data wasn’t available or wasn’t provided for SBE states Idaho, Nevada, and New York. The Center for Medicare and Medicaid Services probably excludes the value to avoid providing an incomplete total. An SBE “total” value isn’t available until 2023.
So we can’t compare 2020 premiums to 2025 premiums as directly as we hoped.
But state-level data is available, so we can compare it that way (except for Idaho, Nevada, and New York):
Average premiums declined for APTC recipients in 26 states.
Average premium after APTC among consumers receiving APTC, 2020 and 2025
In this table, we can at least make an interpretation of how premium costs changed within a state. I emphasize “within” because each state uses a different marketplace platform. That matters because state-based exchanges may offer additional state premium subsidies, not reflected in this federal data.
For that reason, we also can’t make definitive claims from this dataset about true average premiums, just about what the average federal subsidy premium is. And we can’t necessarily make direct comparisons between HC.gov and SBE states, either.
Is the enhancement the only reason we’re talking about subsidies?
Right, let’s get back to the temporary component of the APTC expansion.
Initially, the enhancement was supposed to be through tax year 2022. Then the Inflation Reduction Act of 2022 expanded the provisions through the end of 2025. And because it’s 2026... those enhanced provisions have expired and have returned to the original ACA requirements.
Big Mario is back to little Mario.
But the expiration didn’t happen without notice: the enhanced provisions, and whether to extend them or make them permanent or not, was one of the major conversations during 2025’s government shutdown.
An APTC timeline: Introduction, enhancement, and back.
Although the enhancements expanded eligibility and subsidized premium costs, the subsidies are, well, subsidies and the costs need to be covered by someone — in this case, the federal government.
In FY 2025, premium tax credits and related spending was $140 billion, or doing some back-of-napkin math, roughly 2.00% of the 2025 federal spending.
Near the end of 2025, the Congressional Budget Office (CBO) and the Joint Committee on Taxation estimated that extending the expansion would, by 2035, increase the number of people in the nation with health insurance by 3.8 million and raise the federal deficit by $350 billion.
So, although millions of people did receive subsidies under the temporary expansions, and although Congress did consider what it would take to continue to fund subsidies, they ultimately expired as planned.
As of February 2026, without the enhanced subsidies, CBO estimates that premium tax credits and related spending for FY 2026 will be $117 billion, or roughly 16.4% less than in 2025.
There you have it: everything you need to know about what ACA subsidies are, why they were temporarily expanded, why they expired, and whether you agree with Congress’ decision.